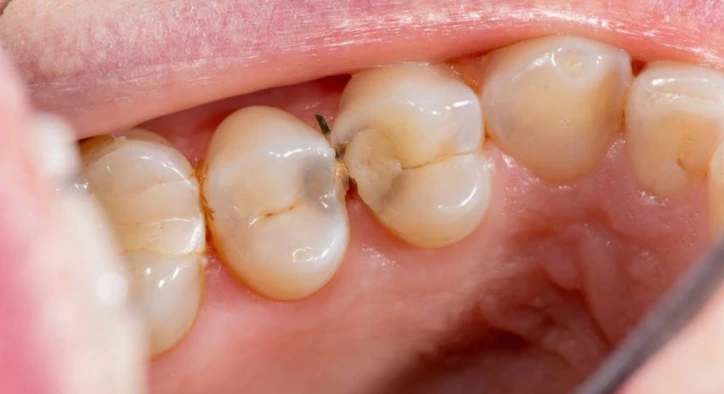
Tooth Decay and a Hole (Cavity): Differences and Treatment Options
Gülüşünüzü ertelemeyin. Uzman hekimlerimizle tedavi seçeneklerini görüşmek için hemen yazın.
WhatsAppTooth Decay is something many people first notice as “just a small spot,” yet it’s actually a dynamic process shaped by tooth chemistry, the oral microbiome, and everyday habits. Over time, it may move from enamel into dentin and, in some cases, toward the pulp. Sometimes it grows quietly; other times it announces itself with sudden sensitivity to hot or cold. So are “decay” and a “hole” (cavity) the same thing, or is one the result of the other?
İçindekiler
- What is Tooth Decay, and what does “cavity” mean?
- How Tooth Decay develops: the oral ecosystem and the acid cycle
- Tooth Decay symptoms: does it always hurt?
- Tooth Decay assessment: what do dentists look for, and which tools are used?
- Tooth Decay treatment options: early stage, cavities, and deeper lesions
- Tooth Decay risk factors: why are some people more prone?
- Living with Tooth Decay risk: the science of prevention and everyday habits
- Why separating Tooth Decay from a cavity matters
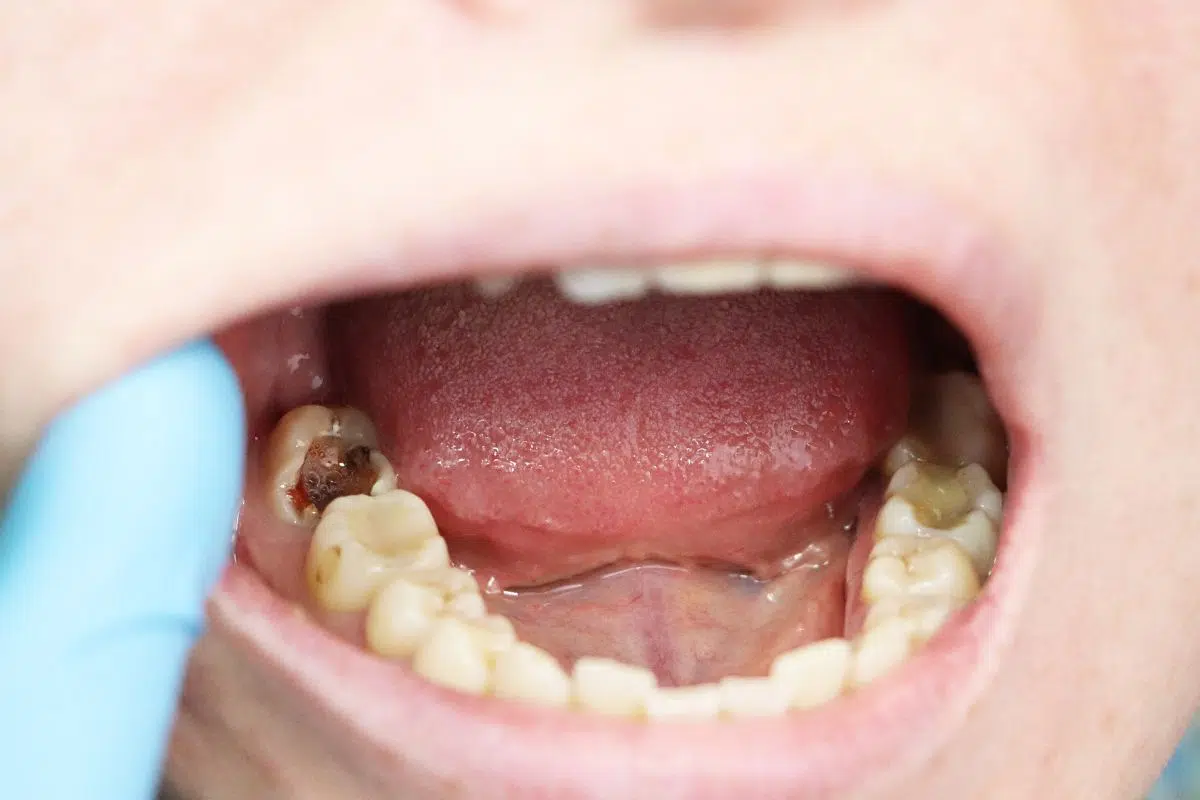
What is Tooth Decay, and what does “cavity” mean?
Tooth Decay is broadly described as the gradual loss of minerals from the hard tissues of the tooth due to acid exposure, weakening the tooth’s structure. The key word here is “process.” Decay usually doesn’t happen overnight. It can begin as microscopic mineral loss in enamel and if conditions allow progress into a visible lesion.
A cavity is typically used to describe the stage where that process results in a visible breakdown of the surface, creating a physical “hole.” In other words, not every case of Tooth Decay has to be a cavity. In early stages, there may be a discussion about potential reversibility (for example, early enamel demineralization). Once a cavity forms, the approach often changes because the tooth has lost structure in a way that can’t simply “close” on its own.
Location also matters. Tooth Decay can appear in pits and fissures on chewing surfaces, between teeth, or near the gumline. A cavity is the point where that area has weakened enough to collapse, leaving a defect that tends to trap plaque and food more easily.
How Tooth Decay develops: the oral ecosystem and the acid cycle
When people hear Tooth Decay, they think “sugar,” and yes sugars are an important piece. But the full story is biochemical. Bacteria naturally living in the mouth metabolize carbohydrates (including sugars and starch-derived carbs) and produce acids. Those acids can pull minerals out of enamel (notably from hydroxyapatite crystals). Put simply: your teeth experience repeated “acid attacks” throughout the day.
What matters is how often and how long those attacks happen. Frequent snacking can extend the time your mouth stays acidic. Saliva is the balancing hero: it helps buffer acids, supports mineral recovery, and keeps the environment more stable. That’s why reduced saliva flow and dryness are often discussed as factors that may influence Tooth Decay risk.
Dental plaque biofilm is the main stage where this happens. The thicker and more mature the plaque, the longer acids can sit against the tooth surface. So Tooth Decay is not only about “sugar”; it’s a combined equation involving bacteria, saliva, tooth anatomy, habits, and sometimes broader health factors.
For a high-level overview of oral health and disease burden, the World Health Organization’s oral health topic page is a useful reference: World Health Organization oral health
Tooth Decay symptoms: does it always hurt?
Tooth Decay doesn’t always start with pain. In fact, early lesions can progress without any noticeable sensation. That’s one of the trickiest parts: decay may advance quietly and only become obvious once a cavity has already formed.
Still, there can be clues. Early enamel demineralization may show as a chalky white, opaque spot. This appearance is linked to how a demineralized surface reflects light differently. When dentin becomes involved, discoloration may deepen—brown shades or shadowing can appear. Tooth Decay between teeth is particularly good at hiding from a mirror, which is one reason radiographs can be helpful in certain evaluations.
Sensitivity depends on the layer affected. Enamel has no nerves, so Tooth Decay limited to enamel may not produce pain. As decay approaches dentin and the pulp, cold or sweet sensitivity, discomfort on biting, or even spontaneous pain may become more likely. However, the absence of pain doesn’t automatically mean “no problem,” because some lesions remain silent until they’re quite advanced.

Tooth Decay assessment: what do dentists look for, and which tools are used?
Assessing Tooth Decay typically isn’t based on a single method. Dentists often combine clinical examination, risk assessment, and imaging when appropriate. They may look at color changes, surface integrity, plaque accumulation, pits and fissures, and gumline areas. Patient-related factors daily cleaning routines, eating patterns, dry mouth complaints often become part of the bigger picture.
On the imaging side, bitewing radiographs are commonly discussed, especially for detecting Tooth Decay between teeth. In some cases, additional angles or tools may be considered. The goal is not only “is it there?” but also “how deep and extensive might it be?”
The table below summarizes common findings and general interpretations (it’s for understanding concepts, not for self-diagnosis):
| Finding | Possible meaning for Tooth Decay | Common areas |
|---|---|---|
| Chalky white spot | Early demineralization, initial lesion | Gumline, around braces |
| Brown shadowing | More advanced lesion, possible dentin involvement | Fissures, between teeth |
| Catching/roughness or surface breakdown | Possible cavity formation | Chewing surface pits/fissures |
| Cold/sweet sensitivity | Possible dentin involvement or near-pulp lesion | Cervical areas, larger lesions |
For foundational, public-health oriented information on cavities and prevention, the CDC oral health pages offer a clear overview: CDC Oral Health
Tooth Decay treatment options: early stage, cavities, and deeper lesions
Treatment planning for Tooth Decay often depends on the stage of the lesion. In early stages, the focus may be on slowing mineral loss and shifting the environment to be less “decay-friendly.” Depending on individual circumstances, this might include professional cleaning, topical fluoride strategies, and improved interproximal (between-teeth) hygiene. The underlying idea is that if the surface has not broken down, the biology of the mouth may support stabilization or partial repair through remineralization under professional guidance.
Once a cavity forms, the situation changes because physical tooth structure has been lost. That defect can become a more plaque-retentive area and may be hard to clean effectively. At that point, restorative options typically come into the discussion fillings, inlays/onlays, or other restorations depending on size and location. The choice is influenced by lesion extent, tooth position, biting forces, aesthetic expectations, and hygiene patterns.
With deeper Tooth Decay, the pulp may be affected. In such cases, endodontic options like root canal treatment may be considered. If structure loss is extensive, a crown may be discussed. Importantly, there isn’t always a single “best” treatment for everyone; planning is usually individualized.
Tooth Decay risk factors: why are some people more prone?
Tooth Decay risk is often the result of multiple factors working together. Some people feel they do everything “right” and still experience repeated issues; others seem to have fewer problems with less consistent routines. That difference isn’t always explained by brushing frequency alone.
Commonly discussed risk variables include:
-
Diet frequency and composition
Frequent intake of sugary or starchy foods can increase the number and duration of acid episodes. Sticky foods may remain on surfaces longer. -
Saliva flow and dry mouth
Saliva supports buffering and remineralization. Certain medications or health conditions can be associated with dryness. -
Plaque control and between-teeth cleaning
Tooth Decay often develops interproximally, so brushing alone may not address all sites effectively. Floss or interdental brushes can be part of the broader conversation. -
Tooth alignment and existing restorations
Crowding, grooves, and restoration margins can create plaque-retentive niches.
These are not “destiny” factors; they mainly help explain why risk differs from person to person and why a comprehensive evaluation can be useful.
Living with Tooth Decay risk: the science of prevention and everyday habits
It can be more realistic to think of Tooth Decay prevention not as a single magic move, but as the accumulated effect of small habits. Decay is sustained by long-term conditions rather than one isolated event.
Frequent snacking can increase total acid exposure time. Sipping sweet drinks over a long period can stretch the acidic window. On the other hand, consistent plaque control, appropriate use of fluoride products, and professional follow-ups can shift the balance. Details such as technique, duration, cleaning at the gumline, and interdental habits can matter as much as “how many times per day.”
Here’s the scientifically fascinating part: the oral bacterial community is not fixed. Diet and hygiene can influence its composition and behavior. That’s one reason modern dentistry often emphasizes risk-based and preventive approaches alongside restorative care.
Why separating Tooth Decay from a cavity matters
Tooth Decay is a continuum from initial demineralization to more advanced breakdown—while a cavity is often the “structural collapse” point in that continuum. Distinguishing the two can help avoid unnecessary intervention while also supporting timely, appropriate restorative planning when a cavity is present.
From the perspective of Avrupa Sağlık Diş, the goal is typically not only to repair a hole but also to understand the conditions that allowed Tooth Decay to develop. Because if the same environment persists, new lesions may appear. That’s why discussions often include both treatment choices and individual risk factors.