Tooth Discoloration: Causes, Types, and Treatment Options
Gülüşünüzü ertelemeyin. Uzman hekimlerimizle tedavi seçeneklerini görüşmek için hemen yazın.
WhatsAppYou look in the mirror, tilt the light, and there it is: your teeth are not quite the shade they used to be. Tooth discolouration is one of the most common dental concerns that patients raise, not because it hurts, but because it is visible. And visible changes to the smile carry real weight. The tricky part is that tooth colour shifts for many different reasons, and the right approach depends entirely on understanding which one you are dealing with.
Table Of Contents
- What Is Tooth Discolouration? The Science Behind Tooth Colour
- Three Types of Tooth Discolouration: Extrinsic, Intrinsic, and Age-Related
- What Causes Tooth Discolouration? A Closer Look at the Usual Suspects
- When Just One Tooth Goes Dark: Trauma, Root Canals, and What It Means
- How Dentists Evaluate Tooth Colour: Shade Guides, Lighting, and Clinical Assessment
- Treatment Options for Tooth Discolouration: From Cleaning to Cosmetic Dentistry
- Addressing Tooth Discolouration in İstanbul: What Patients from the UK Often Ask
- Can You Prevent Tooth Discolouration? Habits That Actually Help
- Myths About Tooth Whitening That Are Worth Questioning
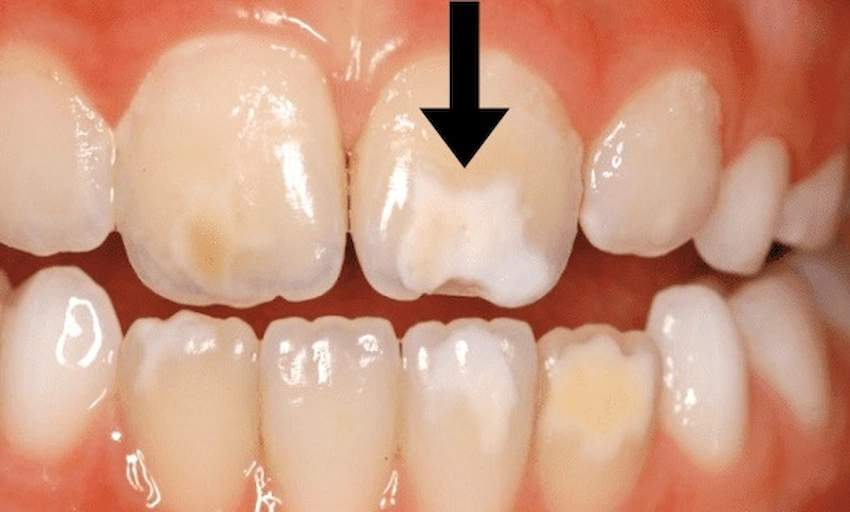
What Is Tooth Discolouration? The Science Behind Tooth Colour
Before exploring how tooth discolouration is treated, it helps to understand why teeth have colour in the first place. Tooth colour is not a simple flat surface shade. It is the result of light interacting with multiple layers: the translucent outer enamel, the naturally yellow-amber dentin beneath it, and the deeper pulp and internal tissue. When light passes through enamel and reflects off the dentin, what you see is an optical blend of all three layers together.
This means tooth discolouration does not always mean something is sitting on the surface. Sometimes the colour change originates inside the tooth structure itself, particularly when enamel thins over time and the dentin becomes more visually dominant. Two people who brush with equal consistency and drink the same morning coffee can end up with quite different tooth shades. Genetics, enamel density, saliva composition, and developmental factors all influence the outcome.
The distinction that matters most clinically is this: did the colour change settle on the tooth, or did it develop within it? That single question shapes almost every treatment decision that follows, which is why a proper assessment matters more than simply choosing a whitening product off the shelf.
Three Types of Tooth Discolouration: Extrinsic, Intrinsic, and Age-Related
Dental research classifies tooth discolouration into three main categories. This classification, well established in peer-reviewed literature including a widely cited review in the British Dental Journal, is genuinely useful because it explains why the same whitening approach works well for one patient and barely shifts the shade for another.
Extrinsic discolouration
This is surface-level staining. Chromogenic compounds from food, drinks, tobacco, and plaque bind to the enamel surface or the thin protein film (pellicle) that coats teeth. Coffee, black tea, red wine, dark berries, soy-based sauces, and tobacco are frequent contributors. Even certain mouthwashes containing chlorhexidine can leave brownish deposits over time with regular use. Extrinsic discolouration tends to respond well to professional cleaning and whitening procedures, though habits need to be addressed alongside treatment.
Intrinsic discolouration
Here, the colour change comes from inside the tooth structure. Causes include physical trauma, root canal treatment with older-generation materials, tetracycline antibiotic use during tooth development, fluorosis from excessive fluoride during childhood, and pulp-related changes. Intrinsic staining often presents as a grey, brown, or bluish tint and cannot be resolved with surface cleaning alone. It requires different approaches, sometimes restorative ones.
Age-related (combined) discolouration
As the years pass, enamel gradually wears and becomes thinner. The dentin underneath, which naturally deepens in colour over time, starts to show through more strongly. This is a biological shift rather than a habit-driven one, and it often combines with years of accumulated surface staining. The result is what many people describe as a general yellowing that creeps up slowly without a clear single cause.
| Type | Primary Source | Appearance | Typical Approach |
| Extrinsic | Diet, tobacco, plaque, certain mouthwashes | Surface spots, lines, general yellowing | Professional cleaning, whitening |
| Intrinsic | Trauma, medications, fluorosis, pulp changes | Grey, blue, or brown tint inside the tooth | Internal whitening or restorative options |
| Age-related | Enamel thinning combined with accumulated staining | General deepening of colour over decades | Whitening or combined restorative approach |
What Causes Tooth Discolouration? A Closer Look at the Usual Suspects
People are often surprised by how many unrelated factors can influence tooth colour. It is rarely one single cause; more often it is several working in combination over years. Knowing where the discolouration originates makes the difference between a treatment that works and one that disappoints.
Dietary habits
The biggest daily contributors are coffee, tea, red wine, and tobacco. These contain tannins and chromogens that adhere to enamel with remarkable persistence. Patients often notice colour returning within weeks of whitening if habits remain unchanged. Rinsing with water after drinking coffee reduces pigment contact time, though it does not eliminate the effect entirely. Dark-coloured fruit juices, soy sauce, and certain curries behave similarly.
Tetracycline and other medications
Tetracycline antibiotics taken during childhood, or by a pregnant mother during tooth development, can bind permanently to developing dentin and cause a characteristic banding pattern ranging from yellow-grey to dark brown. This is one of the most difficult forms of intrinsic staining to address. Certain antihistamines, antipsychotics, and blood pressure medications have also been associated with tooth discolouration over long-term use.
Fluorosis
Fluoride is essential for healthy enamel, but excessive exposure during the years when teeth are forming, typically from unusually high fluoride in water or from swallowing fluoride toothpaste in early childhood, can cause fluorosis. This appears as white streaks or chalky patches in mild cases and brownish discolouration or pitting in more severe ones.
Childhood illnesses and developmental factors
High fevers during infancy, premature birth, or certain disruptions during the period when enamel is mineralising can leave structural changes visible as white patches, opaque spots, or brownish areas. Molar-incisor hypomineralisation (MIH) is one such condition, now recognised as increasingly common. These developmental stains do not respond to conventional whitening because they are structural rather than surface-related.
Plaque and tartar
Plaque is not just a cavity risk. When it mineralises into tartar (calculus), it takes on a yellowish to dark brown appearance that regular brushing alone cannot remove. Tartar-related discolouration is particularly noticeable near the gumline. Regular professional cleaning resolves it, but without periodic removal, tartar accumulates steadily regardless of brushing habits.
Age
This applies to everyone to some degree. Over decades, enamel thins, dentin naturally darkens, and the overall shade shifts towards yellow or grey. This is a gradual biological process, not a sign of poor hygiene. Good oral hygiene can slow the pace of change, but it cannot stop the underlying biology entirely.
When Just One Tooth Goes Dark: Trauma, Root Canals, and What It Means
When tooth discolouration affects only a single tooth, patients typically become more concerned. It makes sense: one tooth standing out from its neighbours is visually striking, and it tends to feel like a signal of something more serious beneath the surface.
The most common cause is previous trauma. A knock to the mouth, a sporting accident, or a childhood fall can trigger internal bleeding within the tooth. Blood products migrate into the dentinal tubules and gradually produce a grey, brown, or pinkish discolouration. This change can appear weeks or even months after the original injury, which sometimes makes it difficult to connect the colour change to its cause. Patients often do not recall the specific incident.
Root canal treatment, particularly when carried out a number of years ago, can also leave a tooth looking noticeably different from its neighbours. Older materials used in endodontics sometimes contributed to internal colour change over time. Modern root canal techniques and sealant materials are significantly better at preserving tooth colour, but older work does not always hold its appearance through the years.
A key nuance: a single darkening tooth does not automatically mean the tooth is unhealthy now. But the "why only this one?" question makes clinical evaluation genuinely worthwhile. If the discolouration is accompanied by sensitivity, swelling near the gumline, or pain on biting, those are signals that warrant prompt assessment. Where the tooth is structurally sound, aesthetic solutions such as internal bleaching or covering with a porcelain restoration can address the colour change very effectively.

How Dentists Evaluate Tooth Colour: Shade Guides, Lighting, and Clinical Assessment
One thing that surprises many patients is how technically involved tooth colour assessment is in clinical practice. The goal is not to decide whether teeth are "white enough", but to understand the baseline shade, the nature and extent of the discolouration, and what realistic treatment outcomes look like before any work begins.
Shade guides, such as the widely used Vita Classical system, provide a standardised reference. Teeth are matched under consistent, controlled lighting using a neutral background. Phone cameras and bathroom mirrors are notoriously unreliable for shade assessment: automatic white balance, warm versus cool light sources, and image compression all distort colour in ways that make self-comparison misleading. Patients who bring in photos from years ago and ask to return to "that shade" are often comparing images taken under very different conditions.
Clinicians also note where on the tooth the discolouration is concentrated. Colour tends to be more intense at the cervical (gum) area and lighter at the incisal edges, partly because enamel is thinner near the gumline and dentin shows through more readily. This spatial variation can make discolouration look uneven even when the underlying cause is uniform.
For cosmetic work, shade assessment must also consider neighbouring teeth, the patient's skin tone, and the lighting conditions the patient lives in, not just the clinical environment. A good colour match in a dental surgery can look slightly off in different light. This is why shade decisions for veneers or crowns involve careful discussion and sometimes trial restorations before final materials are committed to.
Treatment Options for Tooth Discolouration: From Cleaning to Cosmetic Dentistry
There is no single universal treatment for tooth discolouration. The approach depends on the type and origin of the colour change. Once that is established, the available options become clearer and the expectations more realistic.
Professional scaling and polishing
For surface staining driven by diet, tobacco, or tartar build-up, professional cleaning often reveals a considerably brighter shade than the patient expected. Many people are genuinely surprised by the result of their first thorough professional clean after years without one. This step also matters practically: attempting whitening on teeth coated in plaque or tartar reduces its effectiveness and may produce patchy, uneven results.
Teeth whitening (bleaching)
Professional teeth whitening uses hydrogen peroxide or carbamide peroxide to penetrate enamel and break down chromogenic compounds within the dentin layer. In-office procedures produce results within a single session; at-home tray-based methods work over days or weeks. The two approaches are often combined for the most sustained result. Whitening works well on extrinsic staining and some forms of age-related yellowing. It is considerably less predictable for tetracycline staining, fluorosis, and trauma-related intrinsic colour change.
Internal bleaching
This technique is used specifically for non-vital teeth, those that have undergone root canal treatment. A bleaching agent is placed inside the tooth and sealed for a number of days, then renewed until the target colour is achieved. It is a conservative option that avoids the need for full restorative coverage in many cases and is particularly appropriate for single darkened teeth following trauma.
Composite bonding
Dental bonding applies tooth-coloured composite resin directly to the tooth surface to mask discolouration. It is a relatively quick approach, well suited to isolated discoloured areas or single teeth where targeted coverage is more appropriate than full whitening. Results depend on the quality of the composite material and the skill of the clinician applying it.
Laminate veneers and ceramic crowns
For more significant discolouration, particularly in cases where whitening is unlikely to produce sufficient change, laminate veneers or zirconium crowns are frequently discussed. Veneers are thin porcelain or composite shells bonded to the front surface of teeth; crowns provide full coverage. Both options address colour, shape, and minor alignment concerns simultaneously. They represent longer-term solutions but require more preparation and a clear understanding of maintenance expectations.
Microabrasion
Used primarily for fluorosis-related white spots and certain developmental discolourations, microabrasion involves removing a very thin layer of enamel using a mild acid and abrasive combination. It is effective for superficial opaque patches rather than deeper colour changes and is sometimes combined with whitening for improved results.
At Avrupa Saglik Dis, our approach to tooth discolouration starts with understanding which type of staining is present before any treatment is recommended. The goal is not the whitest possible shade; it is the most natural and harmonious result relative to each patient's facial tone and surrounding teeth.
Addressing Tooth Discolouration in İstanbul: What Patients from the UK Often Ask
A significant number of patients travel from the United Kingdom to İstanbul each year for dental treatment, and tooth discolouration is frequently part of the conversation. Many come with a broader plan: a smile design consultation that might include whitening alongside veneers or other cosmetic work. The cost difference compared to UK private dentistry is often considerable, and İstanbul has developed a well-established reputation in this field.
A common concern among UK patients is whether treatment quality abroad matches what they would receive at home. Our dental team includes clinicians with international training and postgraduate qualifications in cosmetic dentistry. Materials used at our clinic come from EU-certified manufacturers, and treatment planning follows the same diagnostic sequence as any reputable European practice: assessment first, realistic outcomes discussed second, treatment third.
Timing is another frequent question. For a consultation, shade assessment, and professional clean, a single appointment is generally sufficient. For whitening, bonding, or veneer work, most patients plan a stay of three to five days. This provides enough time for the dental work and allows for any adjustments before departure. Patients who read through our patient reviews often comment that communication before arrival was clearer than they had expected.
The British Dental Association advises patients seeking treatment abroad to ensure they receive a full diagnostic examination and a clear written treatment plan before any irreversible procedures begin. This is standard practice at our clinic, and we encourage anyone considering treatment to get in touch beforehand so that questions can be answered with proper clinical context rather than general estimates.
Can You Prevent Tooth Discolouration? Habits That Actually Help
Prevention is less exciting than treatment, but it makes a measurable difference over years. The key is consistency rather than dramatic changes.
Drinking coffee or tea through a straw reduces the direct contact time between pigmented liquid and the front surfaces of teeth. It looks unusual, but the logic is sound. Rinsing with water after meals and coloured drinks is a more discreet alternative. Waiting around thirty minutes before brushing after acidic drinks also helps, since enamel is temporarily softened by acid and more vulnerable to abrasion immediately afterwards.
Electric toothbrushes generally remove surface staining more effectively than manual brushing, particularly around the gumline where pigment tends to accumulate. Using a whitening toothpaste is reasonable for maintenance of extrinsic staining, though most whitening toothpastes work via mild abrasion or optical brighteners rather than chemical bleaching. Their effect on intrinsic discolouration is negligible.
Quitting tobacco, in any form, is the single most effective habit change for preventing both extrinsic discolouration and gum disease. Tobacco-related staining is particularly stubborn and penetrates deeper into enamel than food-related pigments. Patients who stop using tobacco almost always notice a meaningful improvement in tooth colour over time.
Regular dental check-ups allow for professional cleaning that removes tartar before it accumulates to a visually significant degree. Most adults benefit from a professional clean every six months; those prone to heavy staining may find more frequent visits worthwhile, particularly if diet or habits are contributing factors.
Myths About Tooth Whitening That Are Worth Questioning
A great deal of misinformation circulates around tooth colour and how to change it. Some myths are harmless; others carry a small but real risk to enamel health.
"Lemon juice whitens teeth." Lemon juice is highly acidic and softens enamel on contact. Any short-term brightness comes from mineral loss rather than stain removal. Regular application erodes enamel permanently and increases sensitivity and cavity risk. This is one of the most persistently recommended home remedies, and one of the most consistently counterproductive.
"Activated charcoal is a safe whitening method." Charcoal-based products are abrasive. They may remove some surface film in the short term, but the abrasive action can roughen enamel over time, creating a surface that holds pigments more readily in future. The evidence base for charcoal as a whitening agent is weak; the evidence for enamel roughening is better documented in the dental literature.
"Whitening works on crowns and veneers." It does not. Bleaching agents only work on natural tooth structure. If natural teeth are whitened after existing crowns or veneers are placed, the restorations remain their original shade while the surrounding teeth lighten, creating a noticeable colour mismatch. Shade matching around existing restorations needs careful planning before any whitening begins.
"Whitening results are permanent." They are not. Staining is a continuous process. Most whitening results begin to fade within months, though the timeline varies considerably depending on diet and habits. Touch-up treatments or at-home maintenance trays are part of a realistic long-term approach rather than an indication that treatment failed.
"All tooth discolouration is the same, so all whitening treatments work equally well." This is perhaps the most clinically significant misconception. Extrinsic staining, intrinsic staining, developmental discolouration, and age-related colour change each respond differently to different approaches. A treatment plan built around the actual type of discolouration present will consistently outperform one based on the appearance alone.
Frequently Asked Questions About Tooth Discolouration
Is tooth discolouration a sign of a dental health problem?
Not always. Surface staining from food, drink, or tobacco is primarily a cosmetic concern. Intrinsic discolouration, however, can sometimes relate to past trauma, previous infections, or developmental factors that benefit from clinical evaluation. A single tooth that turns noticeably darker compared to its neighbours is worth having assessed, even if it causes no discomfort.
Can tooth discolouration return after whitening treatment?
Yes, it typically does over time. Whitening removes accumulated staining but does not prevent new staining from occurring. How quickly it returns depends largely on diet and habits. Some patients maintain results for well over a year with simple adjustments; others see staining return within a few months. At-home maintenance trays can significantly extend the duration of results.
Is teeth whitening safe for people with sensitive teeth?
Sensitivity during or after whitening is common and is usually temporary. For patients with existing sensitivity, a lower-concentration protocol applied over a longer period is often preferred over a single high-intensity session. Using a desensitising toothpaste in the weeks before and after treatment helps many patients manage this. A proper pre-treatment assessment allows the clinician to recommend the most appropriate approach for each individual.
What is the difference between teeth whitening and bleaching?
In dental terminology, "bleaching" refers specifically to treatments that change tooth colour beyond its natural baseline using peroxide-based agents that act on the dentin layer. "Whitening" is a broader term that also includes removing surface staining to restore teeth to their natural shade. Most over-the-counter "whitening" products are doing the latter rather than the former, which is why their results tend to be more modest.
How do veneers differ from whitening for treating discolouration?
Whitening acts on natural tooth structure and works by changing the colour of enamel and underlying dentin. Laminate veneers are thin porcelain or composite shells bonded to the front of teeth, effectively masking the original colour behind a new surface. Veneers are more appropriate when whitening is unlikely to achieve a sufficient result, such as in cases of tetracycline staining, fluorosis, or significant intrinsic colour change. They also improve shape and minor alignment concerns simultaneously, which whitening cannot do.
Can discolouration from tetracycline antibiotics be treated?
Tetracycline-related staining is one of the more challenging forms of intrinsic discolouration to address, partly because it is embedded in the dentin layer and tends to be resistant to conventional whitening. Extended whitening protocols can produce some improvement in milder cases, but more significant staining typically requires restorative solutions such as veneers or ceramic crowns to achieve a natural-looking result. The treatment plan depends on the severity and distribution of the staining.