What is a Dental Abscess and How Does It Heal?
Gülüşünüzü ertelemeyin. Uzman hekimlerimizle tedavi seçeneklerini görüşmek için hemen yazın.
WhatsAppA dental abscess can stop you in your tracks. That sharp, throbbing pain that arrives without warning, the swelling that seems to appear overnight - if you have ever experienced it, you know it is not something you can simply sleep off. A dental abscess is a bacterial infection that leads to a pocket of pus forming either at the root of a tooth or in the surrounding gum tissue. Without treatment, it does not resolve on its own. In fact, leaving a dental abscess untreated can result in serious health complications that extend well beyond your mouth.
This guide covers everything you need to know: what a dental abscess actually is, why it happens, how to recognise one, and what your treatment options look like - including why many patients from across Europe are choosing to have dental abscess treatment in Antalya, Turkey.
Table of Contents
- What Exactly is a Dental Abscess?
- Types of Dental Abscess
- What Causes a Dental Abscess?
- Recognising the Symptoms of a Dental Abscess
- When Should You See a Dentist?
- How is a Dental Abscess Treated?
- Can a Dental Abscess Heal on Its Own?
- How Long Does a Dental Abscess Take to Heal?
- Dental Abscess Treatment in Antalya, Turkey
- Preventing Dental Abscesses
- Dental Abscesses and Your General Health
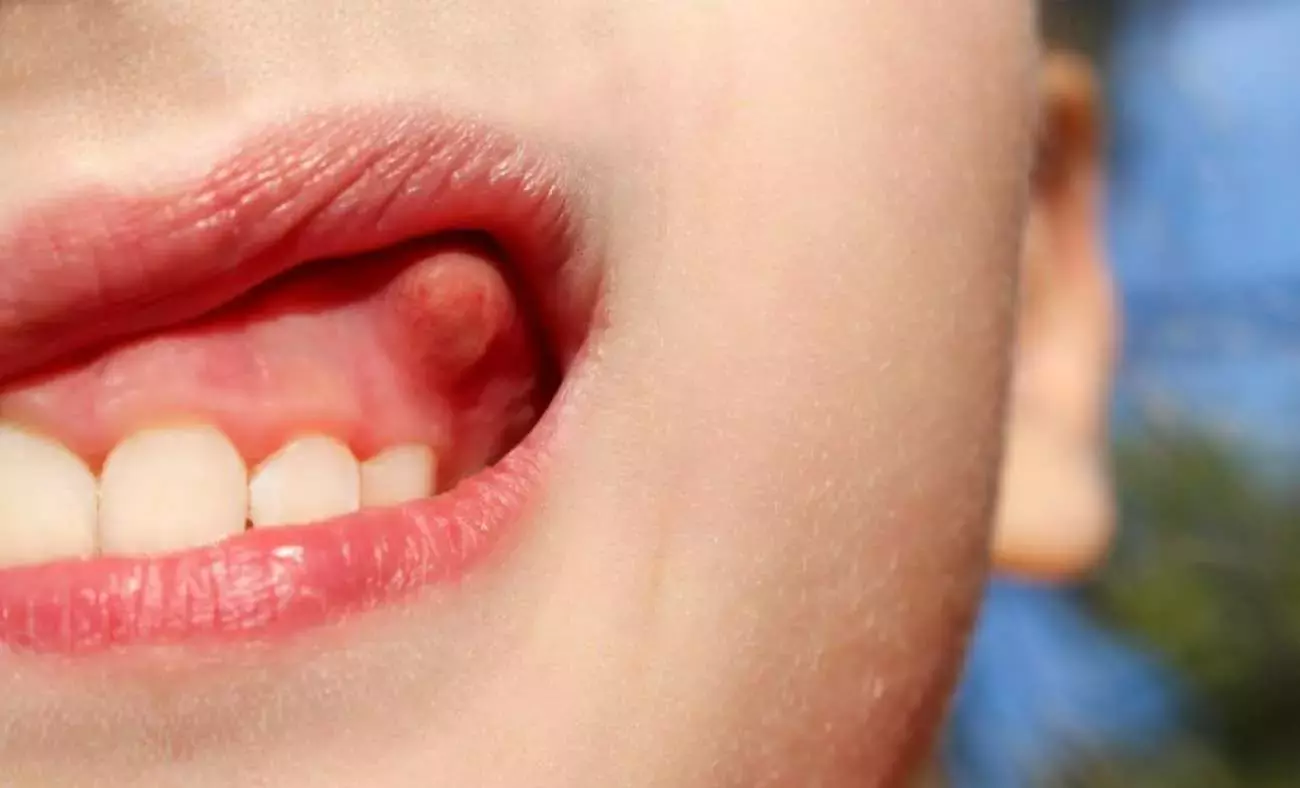
What Exactly is a Dental Abscess?
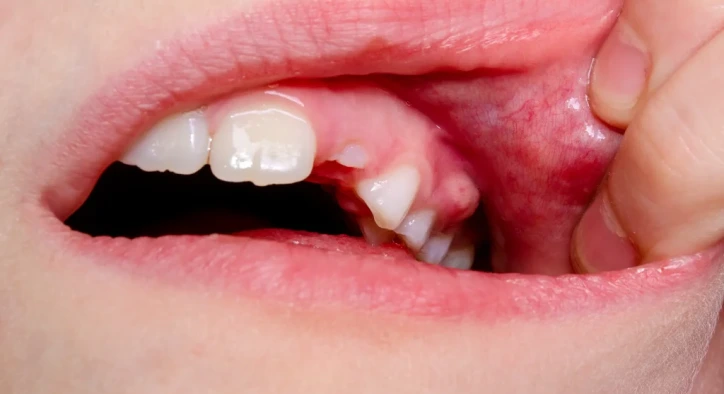
A dental abscess is a collection of pus - a thick fluid made up of dead bacteria, tissue debris, and white blood cells - that forms as a result of a bacterial infection inside or around a tooth. The NHS describes it as "a build-up of pus in the teeth or gums caused by an infection." That pus has to go somewhere, and because it cannot drain naturally, pressure builds beneath the gum or bone, creating the intense pain that many patients describe as the worst toothache of their lives.
Dental abscesses are more common than many people realise. They can affect adults of any age and develop quickly - sometimes over just a few days - particularly when an existing dental problem like a cavity or cracked tooth goes untreated. Left alone, the infection does not stay contained to the tooth. It can spread to the jaw, neck, and in severe cases, the bloodstream. This is why prompt dental care is always essential.
One important distinction worth understanding from the outset: a dental abscess is not the same as ordinary toothache. It is an active infection that the body cannot clear on its own. No amount of painkillers or home remedies will resolve the underlying problem. Professional dental treatment is the only path to full recovery.
Types of Dental Abscess
Not all dental abscesses are identical. The location of the infection determines what type you have, and that in turn shapes how your dentist will approach treatment.
Periapical Abscess
This is the most common type. It forms at the tip (apex) of the tooth root, usually as a result of deep decay, an untreated cavity, or a cracked tooth that has allowed bacteria to reach the pulp - the soft tissue at the centre of the tooth containing nerves and blood vessels. Once the pulp becomes infected, pus builds up at the root tip and spreads into the surrounding bone. Patients with periapical abscesses often experience severe, constant pain that worsens when biting down.
Periodontal Abscess
This type develops in the gum tissue and supporting structures around the tooth, rather than within the tooth itself. It is closely linked to gum disease (periodontitis). Bacteria become trapped in the deep pockets that form between inflamed gums and teeth, creating ideal conditions for infection. Research published in the Journal of the American Dental Association found that patients with periodontal disease were significantly more likely to develop acute periapical abscesses, with some studies reporting an odds ratio of 46 for abscess formation in patients with existing periodontal conditions.
Gingival Abscess
A gingival abscess is confined to the surface gum tissue and does not involve the tooth root or underlying bone. It can result from a foreign object - a fragment of food, a fish bone, or a popcorn kernel husk - becoming lodged in the gum and triggering localised infection. This type tends to be less severe than the others, but it still requires professional drainage and assessment.
| Type | Location | Main Cause | Primary Treatment |
|---|---|---|---|
| Periapical | Tip of tooth root | Decay, cracked tooth, infected pulp | Root canal treatment |
| Periodontal | Gum and supporting tissue | Gum disease, bacteria in pockets | Periodontal therapy, drainage |
| Gingival | Surface gum tissue | Foreign bodies, localised trauma | Drainage, oral hygiene improvement |
What Causes a Dental Abscess?
The root cause of any dental abscess is bacteria. Specific oral bacteria - particularly Streptococcus and Fusobacterium species - can overwhelm the body's defences when they gain access to areas they should not reach: the tooth pulp, the root tip, or deep gum pockets. Several underlying factors create the conditions for this to happen.
Deep or untreated cavities are the most common pathway. When decay erodes through the enamel and dentine and reaches the pulp, bacteria enter the innermost part of the tooth. The pulp becomes inflamed and eventually dies, and the resulting infection tracks down the root into the surrounding bone.
Cracked or fractured teeth provide bacteria with a direct route into the tooth's interior. Even hairline cracks that are invisible to the naked eye can allow bacteria to penetrate. Patients who grind their teeth at night (bruxism) are particularly vulnerable, as are those who play contact sports without a mouthguard.
Gum disease creates the conditions for periodontal abscesses. As gums recede and pockets deepen, bacteria can reach areas that are impossible to clean with a toothbrush or floss alone.
Failed or delayed dental treatment is a contributing factor that many patients do not consider. A cavity left too long, a crown that no longer fits properly, a cracked filling, or a previous root canal that was not fully successful can all allow bacteria to accumulate and infection to develop.
Weakened immune function reduces the body's ability to contain oral bacteria. Patients with diabetes (particularly poorly controlled diabetes), those undergoing chemotherapy, and those taking immunosuppressant medications are at higher risk. Stress also plays a role - chronic stress suppresses immune response and can tip the balance from manageable bacterial load to active infection.
| Risk Factor | Mechanism |
|---|---|
| Untreated tooth decay | Erosion of enamel allows bacteria to reach the pulp |
| Cracked or fractured teeth | Bacteria penetrate directly into the tooth interior |
| Periodontal disease | Deep gum pockets trap bacteria near the root |
| Poorly fitting dental work | Gaps allow bacteria to accumulate beneath restorations |
| Weakened immune system | The body cannot contain bacterial spread effectively |
| Dry mouth (xerostomia) | Reduced saliva removes a key natural antibacterial defence |
Recognising the Symptoms of a Dental Abscess
The symptoms of a dental abscess tend to be difficult to ignore, though they vary depending on the type of abscess and how advanced the infection has become.
The hallmark symptom is persistent, throbbing tooth pain. Unlike the brief sensitivity of a reactive tooth, this pain is typically constant. Many patients describe it as a deep, pulsating ache that radiates to the jaw, ear, and temple on the affected side, and worsens when lying down - which makes sleep particularly difficult during an active abscess.
Other common signs include:
- Visible swelling in the face, cheek, or jaw - sometimes dramatic and asymmetric
- Tenderness and sensitivity around the affected tooth, particularly to pressure and temperature
- A persistent bad taste in the mouth or foul breath, especially if the abscess has begun to drain
- Swollen lymph nodes beneath the jaw or along the neck
- Fever, chills, and a general sense of being unwell - signs the infection is affecting the whole body
- Difficulty chewing or biting on the affected side
- In some cases, a raised, pimple-like bump on the gum near the affected tooth
That raised bump - called a dental fistula or sinus tract - is the body's attempt to create a drain for the infection. When it ruptures, the intense pain may ease and patients sometimes assume the problem has resolved. This is a trap. The infection is still present and will continue to cause damage unless properly treated.
According to the NHS, a dental abscess may cause your tooth to become "very painful" and your face to swell. If you develop difficulty breathing or swallowing, this requires immediate emergency care at A&E.
When Should You See a Dentist?
As soon as you suspect a dental abscess, contact your dentist and ask for an urgent appointment. Waiting to see whether it improves on its own is not a safe approach - the infection can progress quickly, particularly if your immune system is under any kind of stress.
Most dental practices will prioritise patients with suspected abscesses. If your regular dentist cannot see you on the same day, seek an emergency dental appointment elsewhere. In the UK, you can call NHS 111 for advice and referral to emergency dental services.
Go directly to A&E or call 999 if you experience any of the following:
- Difficulty breathing or swallowing
- Swelling that has reached the eye or is causing vision changes
- High fever (above 38.5 degrees Celsius) combined with severe swelling
- Difficulty opening your mouth (trismus)
- Feeling of confusion, extreme fatigue, or a sense that something is seriously wrong
These signs may indicate that the infection has spread to the spaces of the neck, the floor of the mouth, or - in rare cases - the airway. This is a medical emergency that cannot wait for a dental appointment.
How is a Dental Abscess Treated?
The goal of dental abscess treatment is to eliminate the infection, relieve pain, and preserve the affected tooth wherever possible. Modern dentistry has highly effective tools for all three. The specific approach depends on the type of abscess, how advanced the infection is, and the overall condition of the tooth.
Incision and drainage (I&D) is usually the first step. The dentist makes a small incision in the gum or accesses the abscess through the tooth to allow the pus to drain. This provides rapid, often dramatic pain relief. The area is then irrigated with saline to flush out remaining bacteria.
Root canal treatment is the preferred option when the tooth itself can be saved. The dentist removes the infected pulp from inside the tooth, meticulously cleans and shapes the root canals using rotary instruments, and fills them with a biocompatible material to prevent reinfection. A crown is then placed on the tooth to restore its function and structure. At our clinic in Antalya, root canal procedures are performed with rubber dam isolation as standard - a technique that prevents saliva and bacteria from contaminating the canals during treatment, significantly improving success rates. Read more about our root canal treatment with rubber dam approach.
Tooth extraction becomes necessary when the tooth is too severely damaged by infection or decay to save. Removing the tooth eliminates the source of infection. If the tooth later needs replacing, a dental implant is typically the most effective long-term solution, restoring both function and aesthetics.
Antibiotic therapy plays an important supporting role but cannot treat the abscess on its own. Antibiotics help prevent the infection from spreading and are prescribed when fever, significant swelling, or signs of systemic involvement are present. The American Dental Association is clear that antibiotics should complement - never replace - definitive dental treatment. An abscess that appears to respond to antibiotics will almost always return once the course is finished if the underlying cause has not been addressed.
You can learn more about the full range of abscess treatments we offer at our Antalya clinic.
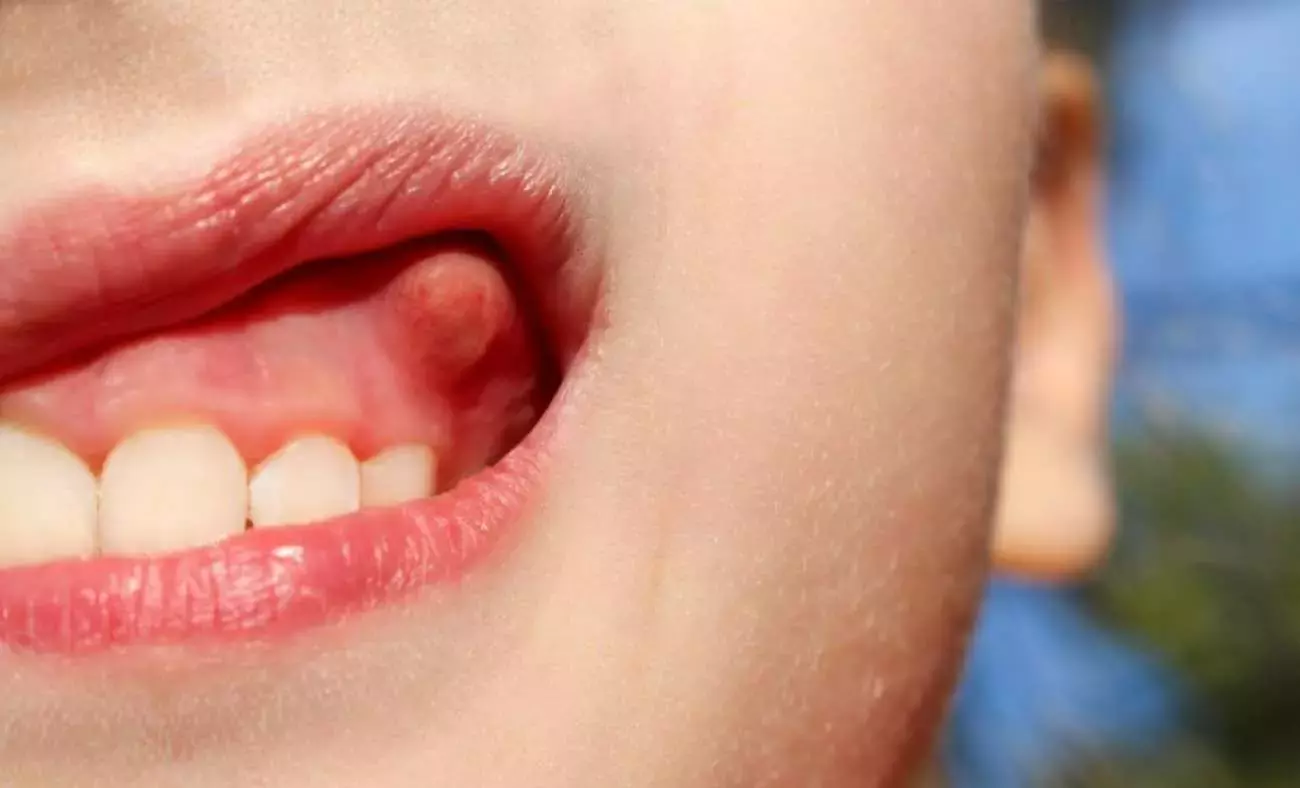
Can a Dental Abscess Heal on Its Own?
No. This question comes up often, and the answer is unambiguous: a dental abscess will not heal without professional treatment. The body cannot clear a tooth root infection the way it might resolve a minor cut or cold. The pus needs to be drained, and the source of the infection - the infected pulp or the bacteria-laden periodontal pocket - needs to be professionally treated.
Home remedies can provide temporary relief while you wait for your dental appointment, and there is nothing wrong with using them for that purpose. Rinsing the mouth with warm salt water several times a day can reduce local inflammation and keep the area clean. Applying a cold compress to the outside of the cheek for 15-20 minutes at a time can bring down swelling and numb the pain. Over-the-counter ibuprofen (an anti-inflammatory) is more effective for dental abscess pain than paracetamol alone.
However, there are several things you should avoid:
- Do not apply heat to the face. Warmth encourages increased blood flow to the area, which can accelerate the spread of infection.
- Do not take someone else's antibiotics. Incomplete antibiotic courses contribute to antibiotic resistance and may mask symptoms without clearing the infection, leading to dangerous delay.
- Do not assume the problem has resolved if the pain eases. This sometimes happens when the abscess drains spontaneously - but the infection is still present and requires treatment.
How Long Does a Dental Abscess Take to Heal?
With prompt and appropriate treatment, most patients experience significant improvement within two to three days. The intense pain typically subsides within 24-48 hours of drainage or root canal treatment. Complete healing - meaning the resolution of all swelling and discomfort - usually takes one to two weeks.
Bone that has been affected by the infection may take longer to regenerate fully. Follow-up X-rays taken three to six months after treatment allow the dentist to confirm that the bone is healing as expected and that no residual infection remains.
The healing timeline varies based on several factors: how quickly treatment was sought, the severity of the infection, the type of treatment performed, and the patient's overall health. Non-smokers and patients with well-managed systemic conditions generally heal faster. Patients with diabetes or those taking immunosuppressants may need closer monitoring during the healing period.
Some post-treatment soreness and mild swelling is normal and usually responds well to over-the-counter painkillers. If your symptoms worsen after treatment, or fail to improve noticeably within five to seven days, return to your dentist. This may indicate the infection is persisting or that further treatment is needed.
Dental Abscess Treatment in Antalya, Turkey
A growing number of patients from the United Kingdom, Germany, and across Europe are choosing to have their dental care - including urgent and complex treatments like abscess management - at specialist clinics in Turkey. Antalya has become one of the leading dental tourism destinations in Europe, and for reasons that go beyond cost alone.
At Avrupa Saglik Dis, our team of experienced dentists and endodontists treats dental abscesses regularly using current clinical protocols. We work with digital X-ray and CBCT imaging for accurate diagnosis, rotary endodontic systems for cleaner root canal procedures, and rubber dam isolation as standard to minimise reinfection risk. Our clinical team is trained to European standards, and the clinic operates under international quality protocols.
For patients travelling from abroad, dental emergencies are rarely convenient. If you develop an abscess before or during a planned trip, or if you have been managing a painful tooth for some time and need proper specialist assessment, we can accommodate urgent appointments. Our team can advise on the most appropriate treatment plan, expected costs, and what to expect during recovery. You are welcome to get in touch via our contact page or find out more about our specialist doctors.
Treatment costs in Turkey are considerably lower than equivalent private care in the UK or Germany - typically 50-70% less for root canal treatment and associated restoration - while accredited clinics maintain standards fully comparable with Western European dental care.
Preventing Dental Abscesses
The good news is that most dental abscesses are preventable. The same habits that protect teeth from cavities and gum disease are the ones that keep abscesses from forming in the first place.
Brush twice daily with a fluoride toothpaste. Fluoride remineralises tooth enamel and disrupts the bacteria that cause decay. Use a soft-bristled brush and spend at least two minutes each time. Replace your toothbrush every three months.
Clean between your teeth every day. Floss or interdental brushes reach the spaces where a toothbrush cannot. Gum disease - and the periodontal abscesses that follow - almost always starts in these gaps. The British Dental Association recommends daily interdental cleaning as a non-negotiable part of oral hygiene.
Attend regular dental check-ups. A dentist can identify cavities and early gum disease well before they progress to the stage where an abscess develops. The recommended frequency varies based on your individual risk profile but is typically every six to twenty-four months.
Act on dental problems early. If your dentist identifies a cavity, do not delay having it filled. If a filling feels loose, a tooth hurts, or a crown does not feel right, have it assessed. Small problems become significant ones quickly - and the difference in treatment complexity and cost between an early filling and an abscess requiring root canal treatment is considerable.
Watch your diet. Frequent consumption of sugary and acidic foods and drinks feeds the bacteria that cause decay. Try to limit these, drink water between meals, and avoid sipping on fizzy drinks throughout the day.
Do not smoke. Smoking is one of the most significant risk factors for gum disease, which in turn increases the risk of periodontal abscesses. It also impairs healing, making treatment outcomes less predictable for smokers than for non-smokers.
Dental Abscesses and Your General Health
A dental abscess is not just a dental problem. The oral cavity and the rest of the body are far more connected than most people appreciate, and an infection that goes untreated in the mouth can have consequences that reach well beyond the teeth and gums.
In severe or prolonged cases, dental infection can spread to the jaw bone (osteomyelitis), the spaces of the neck, or the bloodstream - a condition known as bacteraemia, which can develop into sepsis if not treated. Sepsis is a life-threatening emergency. While this outcome is rare when dental infections are treated promptly, it is not theoretical - case reports of fatalities from untreated dental abscesses continue to appear in the medical literature.
There is also a well-documented relationship between oral health and systemic conditions. Diabetes and dental abscesses have a particularly clear bidirectional link. High blood sugar impairs the immune response and promotes bacterial growth, making diabetic patients more susceptible to oral infections. Conversely, persistent oral infection raises inflammatory markers and can make blood glucose control more difficult. Diabetic patients who experience dental abscesses should always inform both their dentist and their GP or diabetologist.
Research also suggests associations between chronic oral infection and cardiovascular disease. Studies have found elevated rates of coronary heart disease and stroke in patients with untreated periodontal disease, though the causal mechanisms are still being investigated. The working hypothesis involves oral bacteria entering the bloodstream and triggering systemic inflammation.
The NHS states plainly that if a dental abscess is not treated, "the infection can spread to other parts of your body and could make you seriously ill." This is not overstated caution - it reflects genuine clinical risk that justifies treating a dental abscess as urgently as any other acute infection.
Frequently Asked Questions About Dental Abscess
Can I fly with a dental abscess?
Flying with an untreated dental abscess is not recommended. Changes in cabin pressure during flight can significantly intensify tooth pain - a phenomenon sometimes called barodontalgia. The stress of travel may also worsen the infection. If you are travelling to Turkey for dental care, it is sensible to seek initial pain management from a local dentist before flying where possible, and to inform the airline if you are travelling with an acute dental condition. Our team can advise on what to expect and how to prepare for travel.
Is a dental abscess contagious?
The bacteria that cause dental abscesses are naturally present in most people's mouths. The abscess itself is not contagious in the sense that you cannot "catch" one from someone else through casual contact. However, some oral bacteria can be transmitted through saliva - particularly in households with young children. Good oral hygiene for all family members, and avoiding sharing utensils or toothbrushes, reduces this risk.
What happens if I take antibiotics without seeing a dentist?
Antibiotics may temporarily reduce the symptoms of a dental abscess and slow the spread of infection. However, they cannot drain the pus or remove the source of infection - the infected pulp or the bacteria-laden periodontal pocket. Once the antibiotic course finishes, the abscess will almost certainly return. Professional dental treatment is always necessary to resolve a dental abscess. Taking antibiotics without a prescription also contributes to antibiotic resistance, which is a serious public health concern.
Can a wisdom tooth cause a dental abscess?
Yes, and this is relatively common. Partially erupted wisdom teeth are particularly prone to a condition called pericoronitis, where bacteria accumulate under the gum flap partially covering the tooth. This can rapidly develop into an abscess. If a wisdom tooth causes repeated infections, your dentist may recommend extraction. Our team can assess whether this is the appropriate course of action based on the position and condition of the tooth.
How do I know if my toothache is an abscess or just ordinary pain?
A toothache caused by sensitivity or minor decay typically comes and goes, and may be triggered by specific stimuli like hot, cold, or sweet foods. An abscess usually produces constant, throbbing pain that does not ease between episodes and does not fully respond to over-the-counter painkillers. Any toothache accompanied by swelling of the gum or face, fever, a bad taste in the mouth, or swollen lymph nodes should be assessed urgently - these are strong indicators of infection rather than ordinary sensitivity.
Does dental abscess treatment hurt?
The treatment itself should not hurt. Local anaesthesia is used throughout the procedure, and modern anaesthetic techniques are highly effective even in inflamed, infected tissue. The area will feel numb during drainage or root canal treatment, and most patients are surprised by how manageable the experience is compared to the pain of the abscess itself. There is typically some post-procedure soreness for a few days as the tissue heals, but this is well controlled with standard painkillers. Our clinical team at Avrupa Saglik Dis prioritises patient comfort at every stage of the process.