Tooth Loss: Symptoms, Causes, and What to Do
Gülüşünüzü ertelemeyin. Uzman hekimlerimizle tedavi seçeneklerini görüşmek için hemen yazın.
WhatsAppEvery small change in our mouth can trigger a chain reaction that affects the entire body. Especially tooth loss, often seen as a purely aesthetic issue, is actually a complex process that can influence quality of life, eating habits, and even social relationships.
Someone who loses a tooth often thinks it is an isolated event: “One tooth is gone, so what?” Yet every missing tooth in the dental arch can create a domino effect on jaw balance, chewing function, and the position of neighboring teeth. Understanding tooth loss is therefore important not only to grasp current problems, but also to see how further tooth loss might be prevented in the future.
İçindekiler
- What Is Tooth Loss and How Does It Affect the Body?
- Tooth Loss Symptoms: More Than Just a Missing Tooth?
- Causes of Tooth Loss: No Single Culprit
- What Changes in the Mouth After Tooth Loss?
- How Does Tooth Loss Affect Quality of Life?
- Tooth Loss and Preventable Risks: What Can We Control?
- What Can Be Done After Tooth Loss?
- Tooth Loss and the Future: How Should We Position Oral Health?
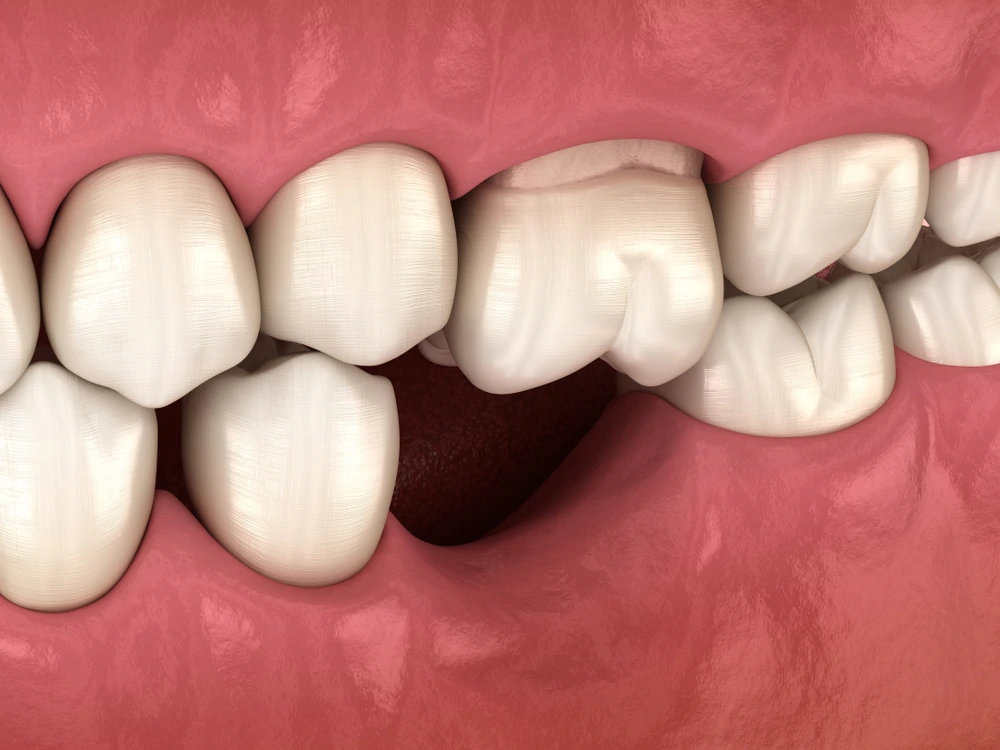
What Is Tooth Loss and How Does It Affect the Body?
In everyday language, tooth loss is usually understood as having a tooth extracted or a tooth falling out on its own. From a clinical perspective, however, the situation is broader. A tooth is a complex structure that extends from the crown to the root, surrounded by bone and gum tissue. Damage to any part of this structure may have consequences beyond the mouth itself.
In areas where a tooth is lost, reduced chewing pressure can gradually lead to loss of jawbone volume. This may result in a sunken facial appearance and reduced support for the lips and cheeks. Additionally, studies suggest that people with multiple tooth loss tend to have less varied diets and may consume fewer fibers, proteins, and certain vitamins, which could indirectly affect the digestive system and overall metabolism.
Tooth Loss Symptoms: More Than Just a Missing Tooth?
Many people assume tooth loss only becomes a problem when the tooth is completely gone. In reality, the process that leads to missing teeth usually begins much earlier, with small but meaningful signals. Recognizing those signals may help reduce the risk of more extensive tooth loss later on.
Common early signs that may precede tooth loss include:
- Tendency to chew on only one side
- Sensitivity or pain when eating hard foods
- A feeling that some teeth are loose
- Gum recession, bleeding, or chronic tenderness
- Food getting stuck repeatedly in the same area
- Difficulty pronouncing certain sounds while speaking
- Gradual widening of gaps between teeth seen in the mirror
These signs do not always mean that tooth loss is inevitable. However, if ignored for a long time, they may allow processes in the bone and gum tissue to progress further, making them harder to manage. In particular, loosening of teeth and gum recession are often described in research as indicators of more advanced periodontal breakdown.
Causes of Tooth Loss: No Single Culprit
When investigating why teeth are lost, focusing on just one factor is rarely enough. In many people, tooth loss develops where genetic predisposition, lifestyle, systemic diseases, and oral hygiene habits intersect. While different studies group the most common causes of adult tooth loss under similar headings, the impact of each factor can vary widely from person to person.
Frequent underlying causes include:
-
Tooth decay (chronic caries processes)
Untreated, long-standing cavities can weaken both the crown and root of the tooth and may ultimately result in extraction. Epidemiological studies often report that a significant proportion of adult tooth loss is related to deep carious lesions involving the root area. -
Periodontal diseases (gum and supporting tissue problems)
Chronic inflammatory conditions affecting the gum and alveolar bone can reduce the support around teeth, causing mobility and eventually tooth loss. Tobacco use, systemic illnesses, and inadequate oral hygiene may accelerate this process. -
Trauma and accidents
Sports injuries, falls, or impacts to the jaw can lead to single or multiple missing teeth. When this happens in the front region, the esthetic and psychological effects often become more obvious. -
Planned extractions in orthodontic or prosthetic treatment
In some complex orthodontic treatments, teeth may be intentionally extracted to align the dental arch. While this is not an uncontrolled tooth loss, it still increases the number of missing teeth and may alter the functional balance of the mouth. -
Systemic diseases and medication
Some chronic conditions (such as diabetes) and certain medications are reported to indirectly affect gum and bone health. When combined with other risk factors, they may increase the likelihood of tooth loss.
Each of these can contribute to the development of tooth loss either alone or in combination. For example, a person who smokes, eats irregularly, and rarely visits a dentist may show a broader and more complex risk profile than someone who does not share those factors.
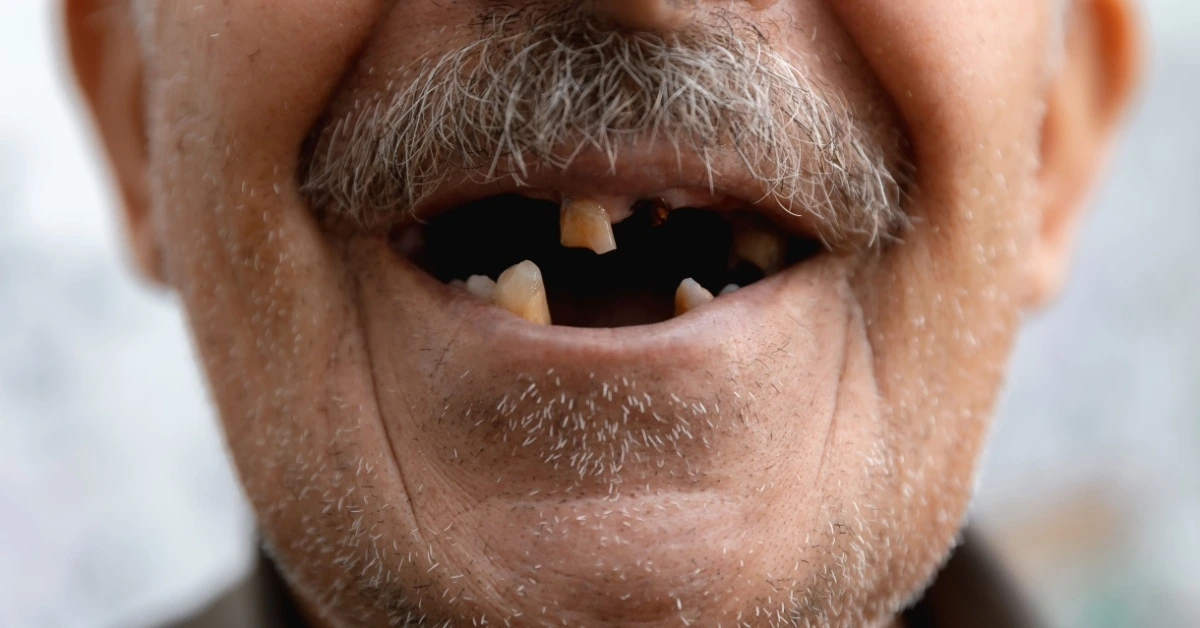
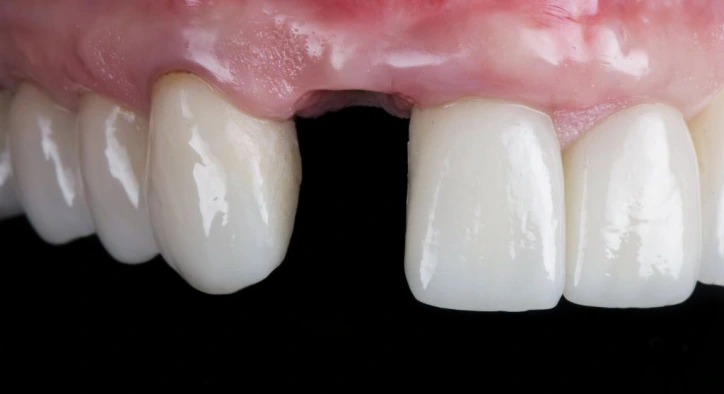
What Changes in the Mouth After Tooth Loss?
At first glance, tooth loss might seem like just an “empty space.” Over the medium and long term, however, missing teeth can trigger a series of structural changes in the mouth. The dental arch is a dynamic system: every tooth affects neighboring teeth, the opposing teeth in the other jaw, and the chewing muscles.
Commonly described changes after a missing tooth include:
- Neighboring teeth tilting into the empty space
- The tooth in the opposing jaw over-erupting toward the gap
- Chewing forces becoming concentrated on certain teeth
- Increased sensitivity or fracture risk in overloaded areas
- Functional imbalance in the temporomandibular joint (TMJ)
To visualize this more clearly, we can compare different scenarios:
| Situation | Possible Outcomes |
|---|---|
| Single missing tooth | Mild chewing imbalance, tilting of adjacent teeth |
| Multiple missing teeth | Reduced chewing performance, changes in eating patterns |
| Front tooth loss | Speech and esthetic impact, reduced self-confidence |
| Back tooth loss | One-sided chewing, increased stress on the jaw joint |
In some long-term, untreated cases of multiple tooth loss, studies report a tendency for people to prefer softer, more carbohydrate-dense foods, potentially influencing weight, digestion, and metabolic balance. While this does not establish a strict cause-and-effect relationship, it underlines the connection between oral and general health.
How Does Tooth Loss Affect Quality of Life?
One of the most visible effects of tooth loss involves self-expression. People who are missing teeth in the front region often start to cover their mouths when they laugh, avoid taking photos, or feel uneasy speaking in front of others. Over time, these behaviors may influence social relationships, work life, and psychological well-being.
Speech also heavily depends on dental alignment. Proper pronunciation of certain sounds requires precise coordination between tongue, teeth, and palate. When front teeth are missing or reduced, some consonants may become harder to articulate. This may cause those affected by tooth loss to become more cautious when expressing themselves verbally.
From a broader, dynamic perspective, the impact of missing teeth on quality of life can be grouped as follows:
- Changes in esthetics and self-confidence
- Difficulties in speech and pronunciation
- Tendency to withdraw from social interaction
- Reduced chewing efficiency
- Dietary shifts due to avoiding certain foods
Various socio-dental studies suggest that individuals with partial or complete edentulism often rate their quality of life lower than those with intact dentitions. These ratings are, of course, subjective, but the trend is consistent. For this reason, tooth loss is not just a mechanical or esthetic problem; it is also a psychosocial process.
Tooth Loss and Preventable Risks: What Can We Control?
Tooth loss is not always entirely preventable. Genetic predisposition, systemic diseases, or unexpected trauma may fall outside personal control. Still, there are many lifestyle and behavioral factors that may reduce the risk of tooth loss or slow its progression.
Looking at the bigger picture, manageable or modifiable risk factors often include:
- Oral hygiene routine (brushing, interdental cleaning, tongue cleaning)
- Habit of attending regular dental check-ups
- Frequency of consuming sugary and sticky foods
- Use of tobacco products
- Parafunctional habits such as mouth breathing, teeth grinding, nail biting
- Use of protective mouthguards during contact sports
Each of these factors alone may not definitively determine whether tooth loss will occur. However, together they may significantly influence the overall risk profile. For example, a person who both smokes and rarely attends dental check-ups may be more vulnerable to periodontal issues.
For those interested in scientific frameworks, the World Health Organization’s overview of oral health presents the teeth and oral structures as integral to general health, highlighting a multifactorial risk model. Such reports can be informative for understanding the link between oral health and systemic well-being. You can find more information on the WHO oral health page:
https://www.who.int/health-topics/oral-health
What Can Be Done After Tooth Loss?
Once a tooth has been lost, many people immediately ask: “What now?” The steps taken afterward can be important for managing the existing gap and for protecting neighboring teeth. It is crucial to remember there is no single “right path” that fits every person. Jawbone condition, remaining teeth, age, systemic health, and personal expectations all influence the approach.
In general, issues that are evaluated after tooth loss include:
- The position and number of missing teeth
- The volume and density of jawbone
- The health and position of neighboring teeth
- Chewing and speech expectations
- The level of esthetic demand
Academic sources describe a wide array of prosthetic and surgical solutions: fixed or removable dentures, implant-supported restorations, bridges, and more. Each option comes with its own advantages, limitations, and maintenance requirements. For that reason, the path to follow after tooth loss usually becomes clear only after detailed oral examination, radiographic assessment, and discussion of the person’s wishes and priorities.
Advances in implantology and digital dentistry over the last two decades have broadened the range of treatment possibilities. Some clinical studies indicate that well-planned, implant-supported prostheses can provide favorable outcomes in terms of chewing function and patient satisfaction. Interest in such research suggests that management options for tooth loss are increasingly grounded in scientific evidence. For those who want a more academic perspective, searching terms like “tooth loss quality of life” on PubMed can yield numerous research articles:
https://pubmed.ncbi.nlm.nih.gov
Tooth Loss and the Future: How Should We Position Oral Health?
Today’s adults may be experiencing less tooth loss than their parents. Several epidemiological reports suggest that, along with rising awareness of oral health, complete toothlessness has declined in some regions. At the same time, more processed food, stress-related parafunctions, and an aging global population can challenge oral health from other angles.
For individuals trying to build a forward-looking strategy, it may be helpful to regard oral health as an inseparable part of overall health. Missing teeth often turn out to be more than a “local oral event,” affecting nutrition, speech, social interaction, and psychological comfort. When tooth loss is viewed from a holistic health perspective, both understanding and managing it may become easier.
Clinics like Avrupa Sağlık Diş, which bring together experience from different branches of dentistry, aim to incorporate this holistic approach into everyday practice. Looking not only at the missing tooth itself, but also at the entire mouth, habits, and expectations, is seen as important for long‑term oral health. Ultimately, the goal is not simply to “fill the gap,” but to reach a balanced situation where chewing function, esthetics, and comfort are considered together.
Tooth Loss as a Turning Point, Not an Ending
Losing a tooth can be a worrying experience. Yet tooth loss does not have to be the final chapter; it can also be a chance to reassess oral health and reconsider lifestyle choices. Cavities, gum disease, trauma, and systemic conditions all offer valuable clues about what is happening in our mouths and, indirectly, in our bodies.
In this article, we have outlined the process leading to tooth loss, its possible symptoms and causes, its impact on oral and general health, and the questions that typically arise afterward. All of this has been discussed with reference to scientific data while still aiming for clarity and readability. Every person’s mouth, medical history, and expectations are unique. Accordingly, any situation involving tooth loss calls for an individualized evaluation and plan.
At Avrupa Sağlık Diş, our perspective is to view a missing tooth not just as an isolated defect, but as one element within the broader picture of the mouth and overall quality of life. Sharing this perspective, supporting informed decisions, and providing balanced, research-based answers are just as valuable to us as any treatment procedure itself.