What Is a Dental Implant Abutment? Its Role and Importance
Gülüşünüzü ertelemeyin. Uzman hekimlerimizle tedavi seçeneklerini görüşmek için hemen yazın.
WhatsAppA detail that often makes an implant treatment feel truly “complete” is the Dental Implant Abutment. The implant body anchored in the jawbone is mostly invisible; what shapes comfort, function, and appearance is the abutment and the restoration placed on top of it. That’s why a Dental Implant Abutment is not just a connector it’s a key component where durability, gum harmony, and natural-looking esthetics meet.
İçindekiler
- Dental Implant Abutment: What It Is and Where It Sits in the Implant System
- What Does a Dental Implant Abutment Do? (Load, Esthetics, and Soft-Tissue Management)
- Dental Implant Abutment Types: Stock, Angled, Custom, and More
- Dental Implant Abutment Materials: Titanium or Zirconia?
- What Influences Dental Implant Abutment Selection? (Angulation, Gums, Hygiene)
- Dental Implant Abutment and the Screw: Micro-Movement, Loosening, and Design Logic
- How the Dental Implant Abutment Process Typically Moves Forward (Impression, Try-In, Final Restoration)
- Why a Dental Implant Abutment Is “Small Part, Big Impact”
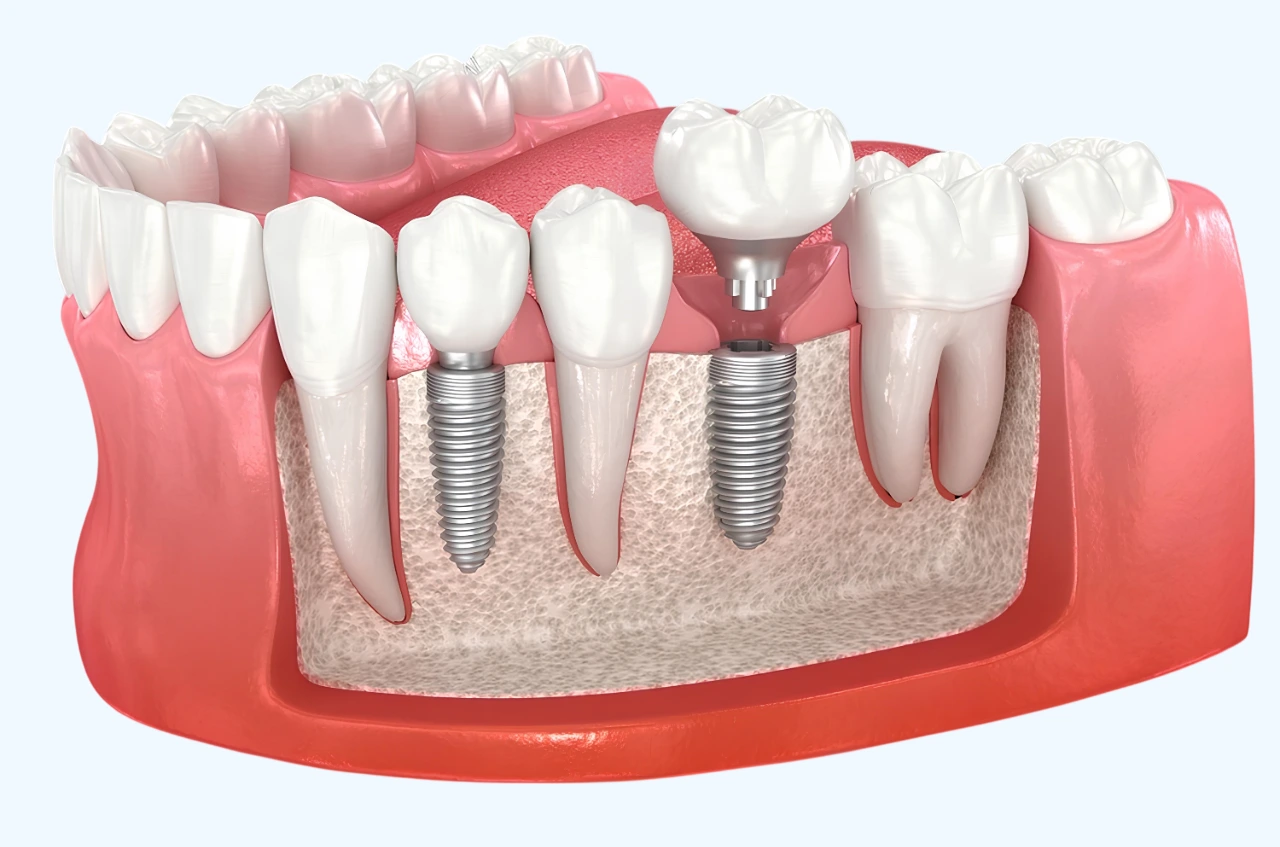
Dental Implant Abutment: What It Is and Where It Sits in the Implant System
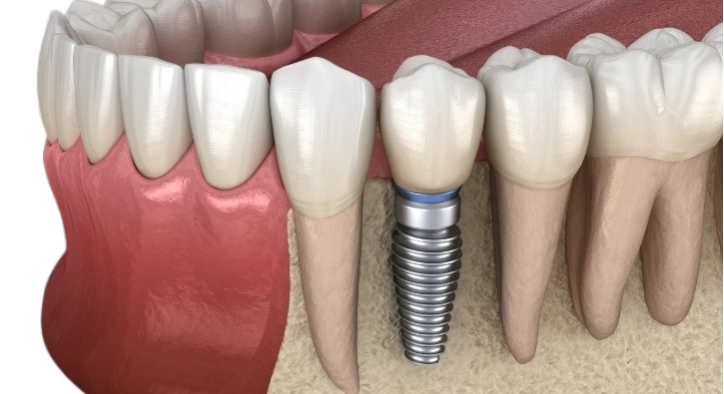
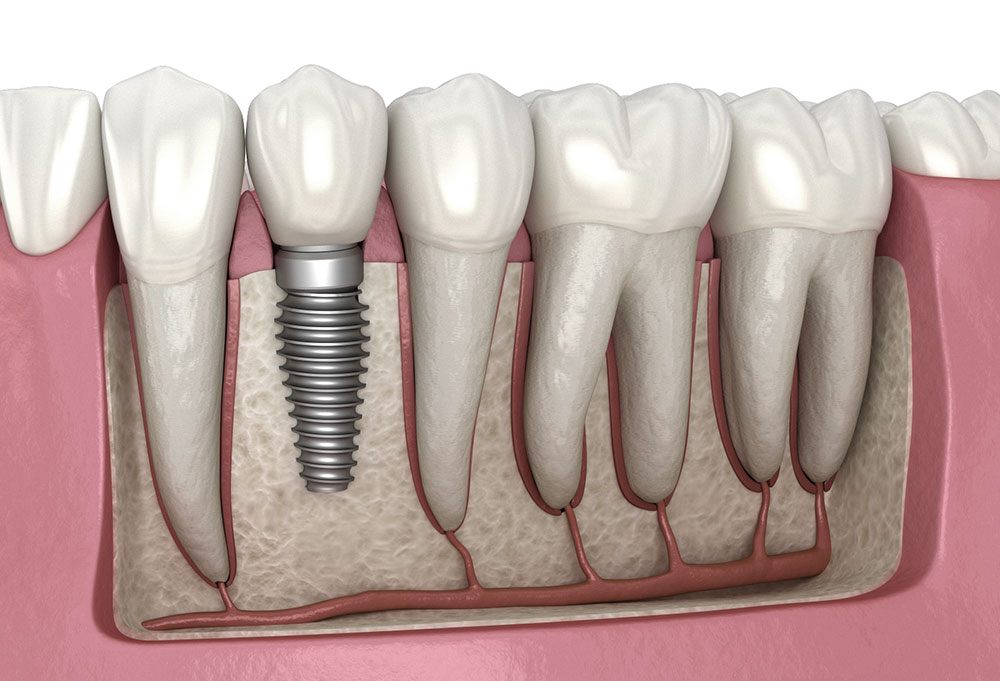
A Dental Implant Abutment is the intermediate component placed between the implant fixture and the visible restoration (a crown, bridge, or denture). Put simply: the implant is the “foundation,” the abutment is the “support column,” and the crown is the “roof.” The harmony of these three strongly influences both mechanical stability and esthetics.
You may see the abutment described as an “implant connector,” “implant superstructure component,” or “implant post.” These are near-synonyms used in clinical communication. Still, Dental Implant Abutment is the clearest umbrella term because it specifies both the implant context and the dental function.
Typically, the abutment is secured to the implant’s internal connection or platform with a defined torque. Then an impression (conventional or digital) is taken and the final restoration is fabricated to sit on that abutment. In some workflows, the abutment and crown can be designed as a unified concept; in others, they remain distinct parts. The choice can depend on esthetic goals, soft-tissue level, implant angulation, and patient-specific functional habits.
What Does a Dental Implant Abutment Do? (Load, Esthetics, and Soft-Tissue Management)
When people hear Dental Implant Abutment, they often think its only job is “to connect.” In reality, it plays multiple roles: transmitting chewing forces, supporting gum contours, and helping the restoration look and feel natural.
The first layer is mechanical. Chewing forces aren’t purely vertical; they include lateral and oblique components. Abutment geometry, connection design, and screw mechanics influence how those forces are transferred into the implant. So abutment selection is not only “Does it fit?” but also “How will it behave over time?”
The second layer is biological. The gumline and surrounding soft tissues form and adapt around the abutment. The surface characteristics, contour, and tissue-contact design can influence cleaning access and perceived tissue compatibility. Different design philosophies exist in the literature and in practice, which is why it’s more realistic to think in terms of “best for this case” rather than one universally “best” option.
The third layer is esthetic. Especially in the anterior region, abutment material and color can affect how light is reflected through thin soft tissue and how lifelike the final crown appears. This is why tooth-colored materials like zirconia may be discussed for certain scenarios while mechanical demands and connection design still remain part of the equation.
Dental Implant Abutment Types: Stock, Angled, Custom, and More
Dental Implant Abutment options come in multiple designs to meet different clinical needs. This variety can look confusing at first, but the goal is straightforward: even if the implant position or angle is less than ideal, the restoration should end up in the right place and orientation.
A practical classification includes:
- Stock (standard) abutments: Manufacturer-made in preset sizes. Often efficient when the case fits the template well.
- Angled abutments: Useful when implant angulation needs correction to improve the restorative path of insertion or screw-channel position.
- Custom (CAD-CAM) abutments: Designed to match the patient’s tissue level, emergence profile, and esthetic targets. Often considered when soft-tissue shaping and precision are priorities.
- Temporary abutments: Used to support provisional restorations; can help guide soft-tissue form during healing and shaping phases.
This overview highlights a key principle: abutments are chosen as part of a restoration plan, not in isolation. For example, a custom design may be selected not because it’s “fancier,” but because it can improve cleansability, support a specific gum contour, or accommodate a unique restorative design.
Abutments can also be discussed in relation to implant connection types (such as internal vs. external connections). Connection geometry can influence load distribution and perceived stability. Instead of broad generalizations, it’s often more accurate to view each implant system as having its own engineering logic and tolerances.
Dental Implant Abutment Materials: Titanium or Zirconia?
When discussing Dental Implant Abutment materials, titanium and zirconia are the most common. Both are widely used, but the choice is usually less about “which is better” and more about “which makes more sense here.”
Titanium abutments have a long history in implant dentistry and are often associated with reliable mechanical performance and extensive clinical experience. Their strengths frequently include durability and stable connection behavior. In highly esthetic zones, especially when soft tissues are thin, clinicians sometimes discuss the possibility of grayish shine-through though the relevance varies from person to person.
Zirconia abutments are often considered for their color advantage, especially in visible areas. If a more natural-looking transition at the gumline is a priority, zirconia’s optical properties can be appealing. Still, factors like design, manufacturing quality, connection concept, and load conditions influence how suitable zirconia is for a given case making case selection an important theme rather than a simple rule.
A quick comparison table can help frame the discussion:
|
Feature |
Titanium Abutment |
Zirconia Abutment |
|
Clinical track record |
Broad, long-standing |
Broad use, but case selection may feel more critical |
|
Esthetics (especially anterior) |
Possible shade influence with very thin tissue |
Often favored for color/optics |
|
Strength perception |
Commonly considered high |
Can vary with design and conditions |
|
Custom CAD-CAM availability |
Yes |
Yes |
This table avoids absolute conclusions because each case has its own “micro-physics.” Still, it reinforces a useful takeaway: color is important, but mechanics and tissue goals matter too.
For readers who enjoy exploring the scientific landscape, these sources provide broad background and searchable research access:
- American Academy of Periodontology: https://www.perio.org/
- PubMed (research database): https://pubmed.ncbi.nlm.nih.gov/
(When you paste this into Word, you can assign these URLs as clickable hyperlinks over the words “American Academy of Periodontology” and “PubMed.”)
What Influences Dental Implant Abutment Selection? (Angulation, Gums, Hygiene)
Choosing a Dental Implant Abutment involves more variables than many people expect. The aim is not only to support a crown, but also to create a setup that remains maintainable over time meaning design can be as influential as material.
One major factor is implant position and angulation. If the implant is not placed along the ideal axis, the restoration’s insertion path (especially in screw-retained designs) may be less favorable. Angled abutments or custom solutions can help relocate the restoration into a more functional and esthetic position.
Another factor is soft-tissue level and thickness. Gum thickness, smile line, and the symmetry of the gum margin can make abutment contouring a high-impact decision. The emergence profile how the restoration “emerges” through the gum can influence the perceived gum shape. Too bulky can make cleaning harder; too narrow can compromise esthetic support. Finding the balance is part of the craft.
Hygiene access matters as well. Many elements affect plaque accumulation around the abutment region: contour, surface finishing, restoration overhangs, and daily cleaning habits. This is why abutment planning and crown/bridge design should be evaluated together; even an excellent abutment can lose its advantages if the final restoration is poorly contoured.
Dental Implant Abutment and the Screw: Micro-Movement, Loosening, and Design Logic
A Dental Implant Abutment is commonly connected to the implant with a screw. It’s a small component with a big job: connection stability influences microscopic movement and the way forces are distributed under function.
One frequently discussed topic is “screw loosening.” This doesn’t automatically indicate poor planning variables like bite forces, parafunction (e.g., clenching/grinding), restorative design, and torque application can all play a role. Connection geometry and abutment design are essentially engineering strategies aimed at improving stability under these conditions.
Another concept is the microgap discussion at the implant–abutment interface. Literature addresses this from multiple angles, and manufacturing tolerances and connection concepts can be relevant. From a patient-friendly standpoint, the practical message is: abutment choice should match the overall implant system and restoration plan, not be treated as a stand-alone decision.
A memorable analogy: think of the abutment screw like the bolts on a high-performance bicycle stem. Tiny, easy to overlook, but if they’re not properly aligned and tightened to specification, comfort and stability can quickly disappear. When everything is engineered and fitted well, the whole system feels solid.
How the Dental Implant Abutment Process Typically Moves Forward (Impression, Try-In, Final Restoration)
The Dental Implant Abutment stage generally comes after the implant has gone through its integration and healing phase. The goal is to preserve soft-tissue health while creating a restoration that sits in the correct position with a suitable contour. Timing and steps can vary, so it’s best viewed as a general flow rather than a single rigid recipe.
In many cases, abutment selection and impression-making are planned together. Digital scans or conventional impressions can be used. Then, in the laboratory workflow, the abutment (chosen as stock or designed as custom) and the final restoration are produced. During try-in visits, fit, contacts, bite relationships, and esthetic integration are evaluated; minor refinements can be made when necessary.
Soft-tissue management is often a quiet star of the process. Temporary restorations or temporary abutments can help guide gum contours into a more ideal form. Gums are not static curtains; they are living tissues that respond to shapes and pressures. This is why subtle contour changes around the abutment area can create noticeable differences in the final esthetic result.
At Avrupa Sağlık Diş, the guiding idea is to align technical precision with esthetic expectations and long-term maintainability. Because every mouth, smile line, and functional habit is different, abutment decisions are typically personalized to the scenario rather than standardized as one-size-fits-all.
Why a Dental Implant Abutment Is “Small Part, Big Impact”
A Dental Implant Abutment is the quiet workhorse of implant dentistry: often unseen, yet highly influential. Load transfer, soft-tissue harmony, esthetic transition, and cleaning convenience are all tied to abutment design and selection. Seeing the abutment as merely a “connector” misses how much it shapes the overall outcome.
In this article, we explored the Dental Implant Abutment through its roles, types, materials, decision factors, and its place in the clinical workflow. The most balanced conclusion is this: there isn’t one universally “best” abutment; there is a best-fit approach guided by goals, anatomy, and functional conditions. In implant dentistry, the results that feel most natural often come from that thoughtful alignment.